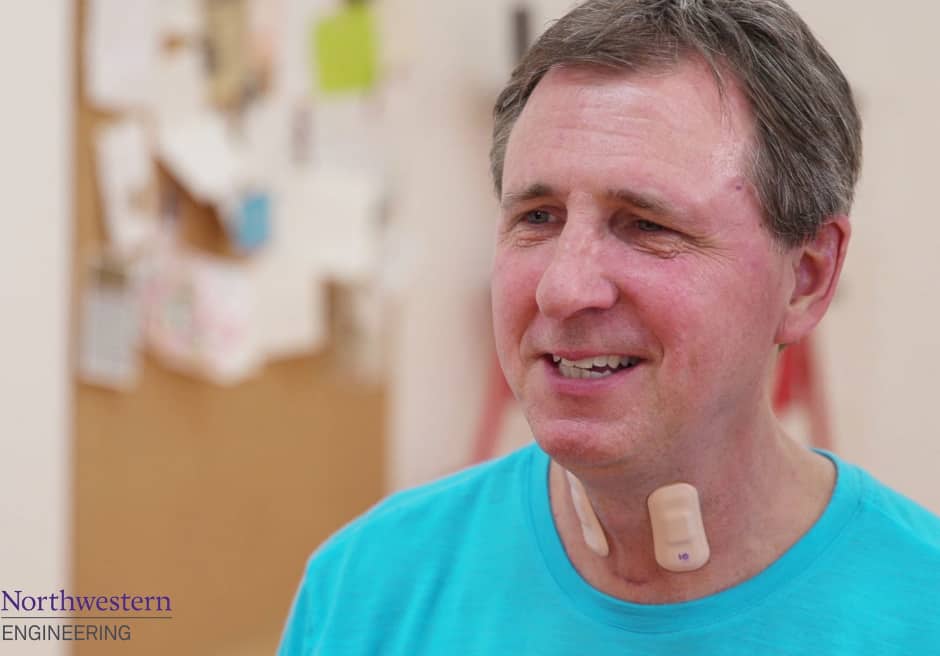
The sensor, developed in the lab of Northwestern University engineering professor John A Rogers, in partnership with Shirley Ryan AbilityLab, joins similar stretchable electronics created by Rogers that can be used in advanced medical care and are portable enough to be worn outside the hospital, even during extreme exercise. The sensors stick directly to the skin, moving with the body and providing detailed health metrics including heart function, muscle activity and quality of sleep.
“Stretchable electronics allow us to see what is going on inside patients’ bodies at a level traditional wearables simply cannot achieve,” Rogers said. “The key is to make them as integrated as possible with the human body.”
Rogers’ new bandage-like throat sensor measures patients’ swallowing ability and patterns of speech. The sensors aid in the diagnosis and treatment of aphasia, a communication disorder associated with stroke.
Tools traditionally used by speech-language therapists to monitor patients’ speech function – such as microphones – cannot distinguish between patients’ voices and ambient noise.
“Our sensors solve that problem by measuring vibrations of the vocal cords,” Rogers said. “But they only work when worn directly on the throat, which is a very sensitive area of the skin. We developed novel materials for this sensor that bend and stretch with the body, minimising discomfort to patients.”
Shirley Ryan AbilityLab, a research hospital in Chicago, uses the throat sensor in conjunction with electronic biosensors on the legs, arms and chest to monitor stroke patients’ recovery progress. The intermodal system of sensors streams data wirelessly to clinicians’ phones and computers, providing a quantitative, full-body picture of patients’ advanced physical and physiological responses in real time.
“One of the biggest problems we face with stroke patients is that their gains tend to drop off when they leave the hospital,” said Arun Jayaraman, a research scientist at the Shirley Ryan AbilityLab. “With the home monitoring enabled by these sensors, we can intervene at the right time, which could lead to better, faster recoveries for patients.”
Because the sensors are wireless, they eliminate barriers posed by traditional health monitoring devices in clinical settings. Patients can wear them after discharge from hospital, allowing doctors to understand how their patients are functioning in the real world.
“Talking with friends and family at home is a completely different dimension from what we do in therapy,” said Leora Cherney, research scientist at the Shirley Ryan AbilityLab and an expert in aphasia treatment. “Having a detailed understanding of patients’ communication habits outside of the clinic helps us develop better strategies with our patients to improve their speaking skills and speed up their recovery process.”

Data from the sensors will be presented in a dashboard that is easy for both clinicians and patients to understand. It will send alerts when patients are underperforming on a certain metric and allow them to set and track progress toward their goals.
Rogers presented research on the implications of stretchable electronics for stroke recovery treatment on Saturday, Feb 17, at the American Association for the Advancement of Science (AAAS) annual meeting in Austin, Texas.









McMurtry Spéirling defies gravity using fan downforce
Ground effect fans were banned from competitive motorsport from the end of the 1978 season following the introduction of Gordon Murray's Brabham...